Active ingredient could restore movement after stroke even days later
Researchers at the Institute for Basic Science (IBS) in South Korea have deciphered a previously unknown mechanism of delayed brain damage after stroke and developed an experimental drug that can stop this process. The drug KDS12025 showed a clear effect in mice and monkeys even when administered up to two days after the event.
Every stroke begins with a sudden interruption of the blood supply. After that, however, a chain reaction begins: Greatly increased hydrogen peroxide (HâOâ) levels cause astrocytes (supporting cells of the brain) to produce massive amounts of type I collagen. This collagen is incorporated into the so-called glial barrier and actively promotes the death of nerve cells â a process that takes days.
The team led by Director C. Justin LEE (Center for Memory and Glioscience, IBS) and Professor RYU Seungjun (Eulji University) was able to show that the targeted inhibition of this mechanism with the new active ingredient KDS12025 prevents collagen production, protects nerve cells and significantly improves motor function.
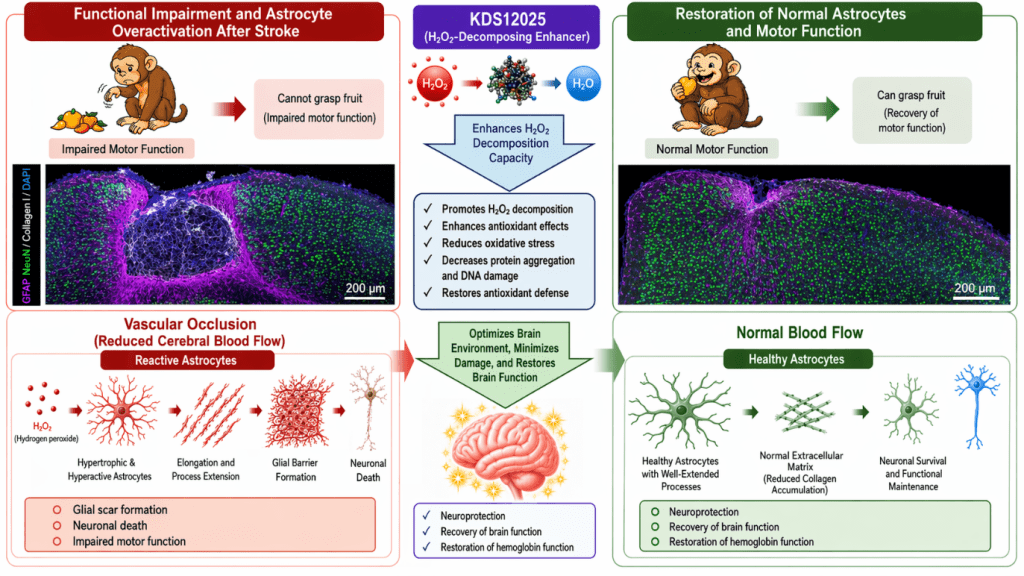
In mouse models, the treatment led to a significant reduction in brain damage. The results in the monkey model were particularly impressive: untreated animals were unable to grasp food due to paralysis, while monkeys treated with KDS12025 were able to access it successfully in all 10 out of 10 experiments.
“Not only did we elucidate the underlying mechanism, but we also developed a concrete therapeutic strategy,” said C. Justin LEE. “The fact that the drug is still effective days after the stroke could significantly expand the therapeutic window.”
The study was published on April 27, 2026 in the journal Cell Metabolism (DOI: 10.1016/j.cmet.2026.04.001). In the long term, the results could also be relevant for other neurodegenerative diseases such as Alzheimer’s or Parkinson’s, in which similar oxidative and inflammatory processes play a role.
Original Paper:
Read Also:
Stem cells repair stroke damage – MedLabPortal
Editor: X-Press JournalistenbÞro GbR
Gender Notice. The personal designations used in this text always refer equally to female, male and diverse persons. Double/triple naming and gendered designations are used for better readability. ected.




