Explainable AI reveals hidden tissue changes in type 2 diabetes
For the first time, a research team has used explainable artificial intelligence (AI) to visualize subtle structural changes in the pancreas of people with type 2 diabetes. The study, in which the German Diabetes Center (DDZ) in Dû¥sseldorf, the Paul Langerhans Institute Dresden and the Institute for Diabetes Research and Metabolic Diseases at the University Hospital Tû¥bingen were significantly involved, is based on an extensive data set of 100 tissue samples from Dresden and Tû¥bingen.
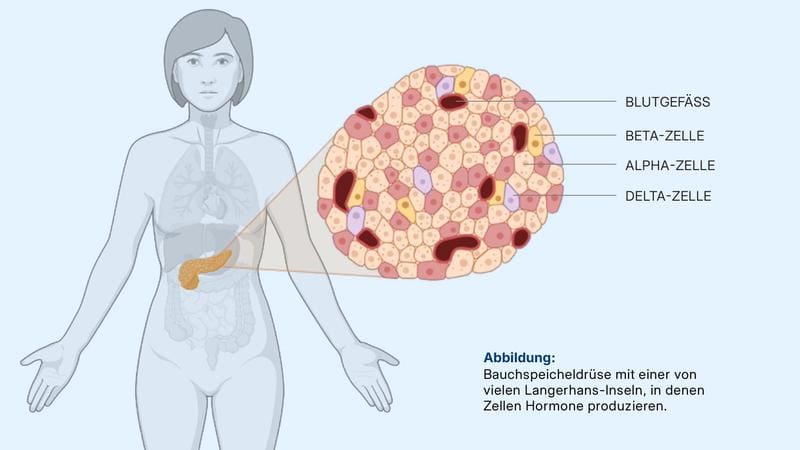
Type 2 diabetes is usually diagnosed via elevated blood glucose levels. However, these mainly reflect the consequences of the disease, not its structural causes in the pancreas. There, the islets of Langerhans with beta, alpha and delta cells as well as surrounding structures such as blood vessels, connective tissue, fat cells and nerve fibers regulate blood sugar levels. Until now, changes in this complex network were often not clearly recognizable under the microscope, as cell composition and arrangement differ greatly from person to person.
The interdisciplinary team used machine learning to train deep learning models on high-resolution whole-section images of the pancreas of operated patients with and without type 2 diabetes. The explainable AI achieved a high predictive accuracy for diabetes status and at the same time marked the crucial image regions that could be further analyzed biologically and statistically.
The results show that it is not only the beta cells that change in type 2 diabetes. Alpha and delta cells also show changed positions and distributions, the islets of Langerhans are smaller overall. Particularly striking is the more frequent proximity of fat cells to the islets, which could impair their function. Neuronal structures and other tissue characteristics also play a role.
The findings also open up new starting points for understanding disease mechanisms and developing targeted therapies. The researchers are making the complete code for image processing, model training and explanatory analyses publicly available in order to further develop the method.
The study has been published in the journal “Nature Communications” (2026 edition). In addition to the aforementioned institutes, other partners from the German Center for Diabetes Research (DZD), the German Cancer Research Center (DKFZ) and international cooperation partners were involved.
Original Paper:
Editor: X-Press Journalistenbû¥ro GbR
Gender Notice. The personal designations used in this text always refer equally to female, male and diverse persons. Double/triple naming and gendered designations are used for better readability. ected.




